Many people believe that pregnancy allows a woman to “eat for two” with no concern regarding weight gain. However, nutrition experts say this is not exactly true.
It is true that weight gain — within limits — is important during pregnancy. Extra calories provide nourishment to your developing baby and are also stored for breastfeeding your baby after delivery. On the other hand, excessive weight gain brings with it a variety of complicated risks. Let’s take a closer look at these factors.
Potential risks from excess weight gain:
- Stillbirth
- Preeclampsia (an abnormal state of pregnancy characterized by hypertension and fluid retention)
- Glucose intolerance
- Cesarean delivery
- Macrosomia (having a large baby for the gestational period)
- Varicose veins
- Difficulty breastfeeding
- Postpartum weight retention
- Childhood obesity in your baby’s future
Potential risks from not gaining enough weight:
Unfortunately, it is not as simple as avoiding weight gain. There are risks associated with not gaining enough weight if you are not overweight before becoming pregnant, including:
- Low birth weight or very low birth weight baby
- Preterm birth
- Neural tube defects
How do you know how much weight is enough to gain?
1. Find your pre-pregnancy Body Mass Index (BMI). Your BMI is a measure of body composition based on height and weight. To calculate your BMI, use the following link: https://www.cdc.gov/nccdphp/dnpa/bmi/, or you can use the following equation:
Weight in kilograms
(Height in meters)2
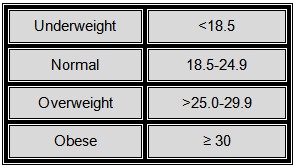
2. After you know your BMI, you can classify your pre-pregnancy weight based on the classifications made by the World Health Organization:
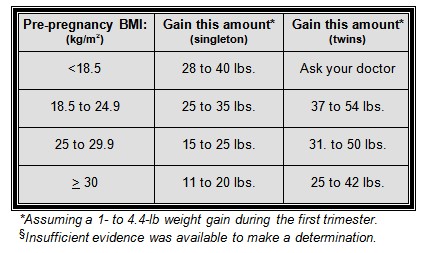
3. Once you know what classification you fall under, you can see how much weight you should plan to gain, based on the Institute of Medicine recommendations:
The Institute of Medicine modified the recommended weight gain range after 19 years. The reason for the new guidelines is that there have been dramatic changes in the population of women having babies. American women are now a more diverse group; they are having more twin and triplet pregnancies, and they tend to be older when they become pregnant. Women today are also heavier; a greater percentage of them are entering pregnancy overweight or obese, and many are gaining too much weight during pregnancy. Many of these changes carry the added burden of chronic disease, which can put the mother and her baby’s health at risk.
Although there is a range of recommended weight gain among women with a BMI of 30 kg/m(2) or higher, some studies have suggested that little or no weight gain is actually associated with better outcomes for obese women and her child. Excess pregnancy weight raises the risk of pregnancy-induced hypertension and diabetes, cesarean sections and birth injuries. Further studies are currently being conducted.
At what rate should you gain during your pregnancy?
This depends on your weight before you were pregnant.
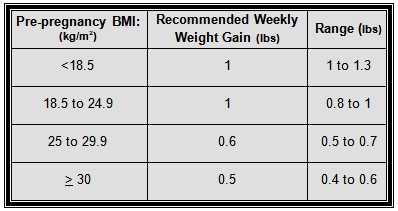
There is no increased energy cost associated with the first trimester of a singleton pregnancy. A weight gain of 1 to 4.5 pounds is acceptable for most women. Recommendations for weight gain during the 2nd and 3rd trimesters are as follows:
How do you gain adequate weight healthfully?
Typically during the first trimester, new recommendations don’t include an increase in calories. Steady weight gain is more important in the second and third trimesters, especially if you began your pregnancy at a normal weight. An extra 340 calories a day is typically enough 2nd trimester and 450 calories extra during the 3rd trimester.
Here’s what 340 calories looks like:
- 1 medium banana with 2 Tablespoons peanut butter
- Half-cup trail mix with nuts, seeds, and dried fruit and half of a small apple
- 12 almonds with 7 oz yogurt and 1 small orange
- 1/3 cup hummus with 7 whole wheat crackers and carrot sticks
- 1 cup milk and 4 fig bars
Here’s what 450 calories looks like, which could be a mid-afternoon mini-meal:
- A a salad with 3 cups mixed greens, ¾ cup low-sodium white beans, drained and rinsed, 1 tablespoon hummus, ½ cup grape tomatoes, ½ cup diced cucumber, 1 1/2 oz. pasteurized feta cheese, 2 teaspoons fresh lemon juice, 1 teaspoon red wine vinegar, 2 teaspoons EVOO, Fresh parsley (1)
- A ½ cup uncooked old-fashioned rolled oats with 2 tablespoons chia seeds, ¾ cup low-fat milk or soy milk, ½ cup fresh or frozen blackberries, 1 tablespoon honey, ½ teaspoon cinnamon (2)
For women who are overweight before pregnancy, increasing daily calories by no more than 100 calories beyond the pre-pregnancy intake appears to be sufficient. Fat should be limited to less than 30 percent of calories and come in the form of “good” unsaturated fats, from sources like nuts, avocados, olive and canola oils.
Some women need more or fewer calories, depending on their individual metabolism and activity level. Make an appointment with a registered dietitian nutritionist. Make sure they have the credentials RD or RDN. In many instances, a doctor can write a referral and a few visits will be covered by insurance. Gradual weight gain is ideal. There is no need to worry if you do not hit the targets mentioned above exactly. The important thing is to pay attention to your overall weight gain and to treat your body in a healthy way. See The ABC’s of Growing a Healthy Baby for more information.
All Nutrition articles were updated November 2017